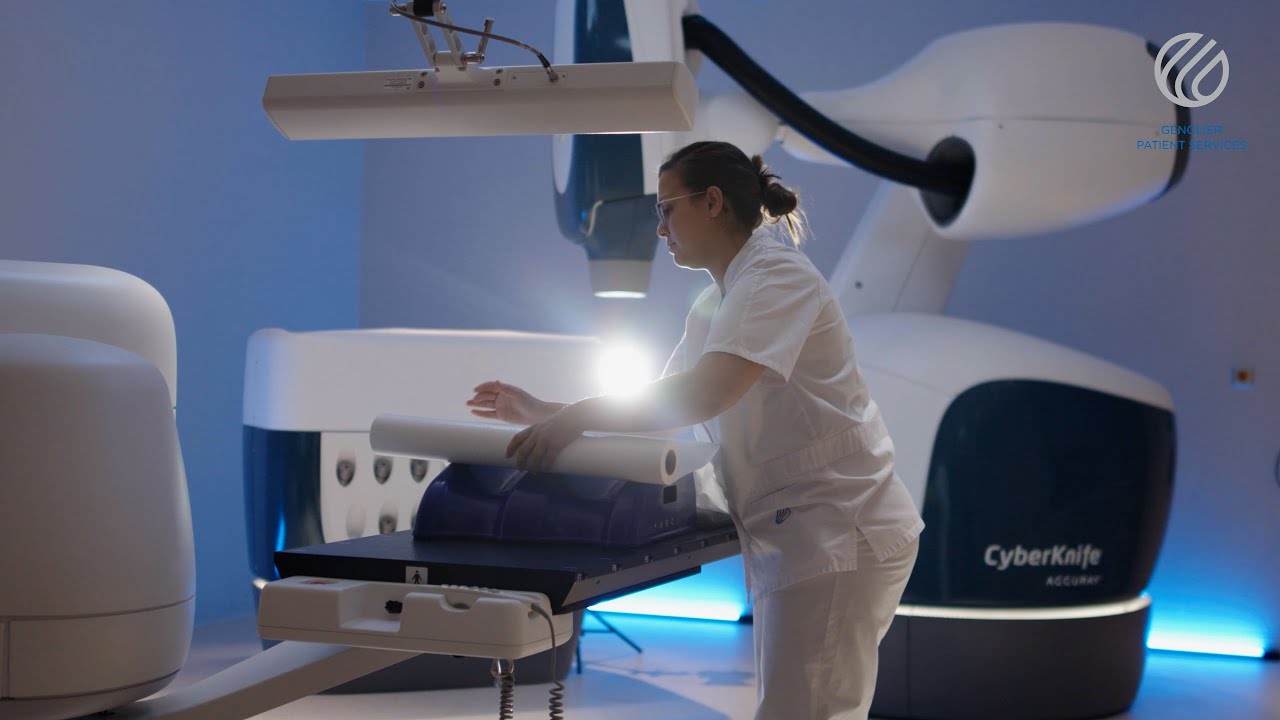
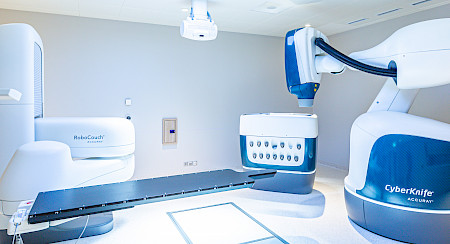
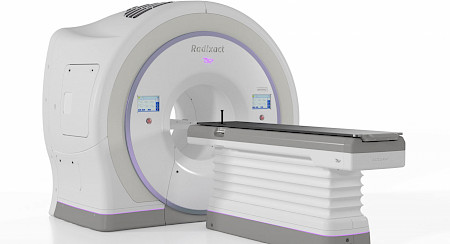
Your treatment in our radio-oncology department follows a request made by your oncologist or specialist. In order to present you with the details of our treatment proposal, you will receive an appointment for a «first consultation». During this consultation, a radio-oncologist from our network will present the indications, benefits and possible side effects of the treatment. He or she will also discuss the various treatment strategies with you and may recommend additional examinations.
-
Hospitals
back
Hospitals
- Clinique de Genolier
- Clinique de Montchoisi - Lausanne
- Clinique de Valère - Sion
- Clinique Générale Ste-Anne - Fribourg
- Clinique Générale-Beaulieu - Geneva
- Clinique Montbrillant - Chaux-de-Fonds
- Clinique Valmont - Glion sur Montreux
- Hôpital de La Providence - Neuchâtel
- Hôpital de Moutier
- Hôpital de Saint-Imier
French-speaking Switzerland -
Centres
back
Centres
- Centre Médical Eaux-Vives
- Centre Médical Valère
- Consultations dans le Haut Valais
- Médicentre Corgémont
- Medicentre Courroux
- Medicentre Courtelary
- Médicentre Moutier
- Médicentre Tavannes
- Medicentre Valbirse
- Montchoisi Medical Center
- Policlinique de Valère
- Polyclinic Genolier
- Ärztezentrum Bümpliz
- Ärztezentrum Ittigen
- Ärztezentrum Oerlikon
- Ärztezentrum Ostermundigen
- Ärztezentrum Schönburg
- Ärztezentrum Siloah Liebefeld
- Ärztezentrum Siloah Murten
- Ärztezentrum Solothurn
- Ladies Permanence Stadelhofen
- Medizinisches Zentrum Biel
- Medizinisches Zentrum Haus zur Pyramide
- Xundheitszentrum
French-speaking SwitzerlandGerman-speaking Switzerland - Swiss Visio
- Medical specialty
- Doctors
-
For patients
- About us
-
Integrated care
-
Hospitals
back
Hospitals
- Clinica Ars Medica - Gravesano
- Clinica Sant'Anna - Sorengo
- Clinique de Genolier
- Clinique de Montchoisi - Lausanne
- Clinique de Valère - Sion
- Clinique Générale Ste-Anne - Fribourg
- Clinique Générale-Beaulieu - Geneva
- Clinique Montbrillant - Chaux-de-Fonds
- Clinique Valmont - Glion sur Montreux
- Hôpital de La Providence - Neuchâtel
- Hôpital de Moutier
- Hôpital de Saint-Imier
- International Patients
- Privatklinik Belair
- Privatklinik Bethanien - Zürich
- Privatklinik Lindberg - Winterthur
- Privatklinik Obach - Solothurn
- Privatklinik Siloah
- Privatklinik Villa im Park, Rothrist
- Rosenklinik Rapperswil
- Schmerzklinik Basel
- Spital Zofingen
-
Centres
back
Centres
- Ars Medica Agno
- Ars Medica Bellinzona
- Ars Medica Manno
- Ärztezentrum Bümpliz
- Ärztezentrum Ittigen
- Ärztezentrum Oerlikon
- Ärztezentrum Ostermundigen
- Ärztezentrum Schönburg
- Ärztezentrum Siloah Liebefeld
- Ärztezentrum Siloah Murten
- Ärztezentrum Solothurn
- Centre Médical Eaux-Vives
- Centre Médical Valère
- Centromedico
- Consultations dans le Haut Valais
- Ladies Permanence Stadelhofen
- Médicentre Corgémont
- Medicentre Courroux
- Medicentre Courtelary
- Médicentre Moutier
- Médicentre Tavannes
- Medicentre Valbirse
- Medicentro Pediatrico
- Medicentro Sant'Anna
- Medizinisches Zentrum Biel
- Medizinisches Zentrum Haus zur Pyramide
- Montchoisi Medical Center
- Policlinique de Valère
- Polyclinic Genolier
- Xundheitszentrum
- Cancer centres
- Radiology centres
- Spine centres
- Sports medicine centres
- Neurology centres
- Centre du Sein
- Swiss Visio
- Medical specialty
- Doctors
-
For patients
back
For patients
- About us
-
Integrated care
close search